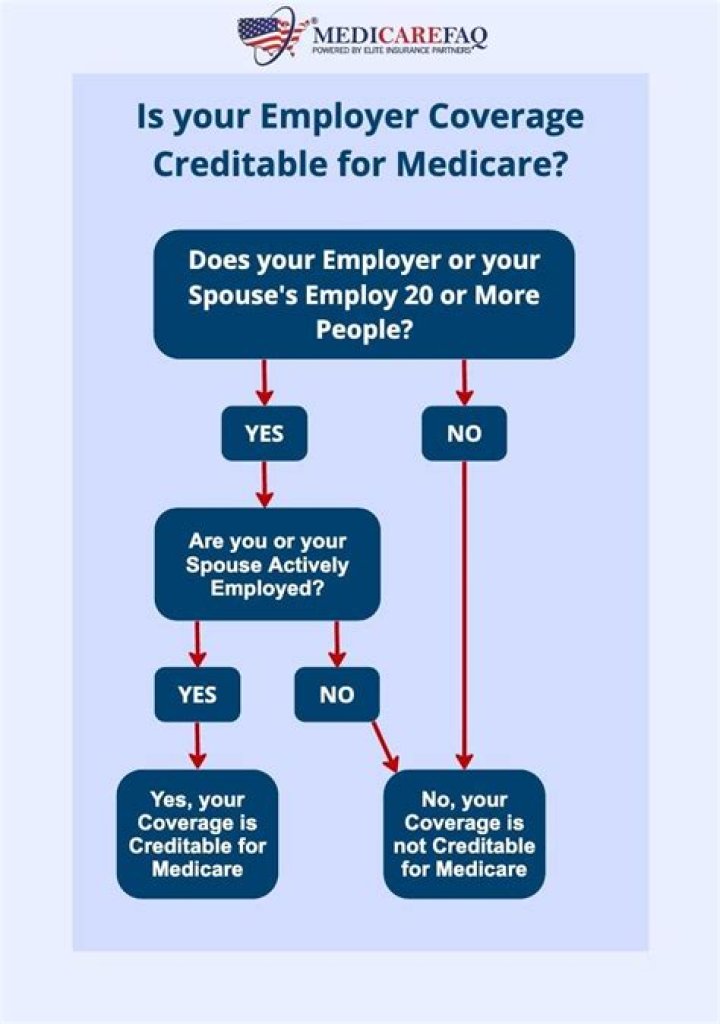
Creditable coverage is defined as health insurance that meets or exceeds what Medicare covers. If you have creditable coverage, you can delay signing up for Medicare without penalty. If you lose your creditable coverage, you must sign up for Medicare within 8 months; otherwise, penalties and late fees may apply.
What qualifies as creditable coverage?
Creditable coverage is a health insurance, prescription drug, or other health benefit plan that meets a minimum set of qualifications. Types of creditable coverage plans include group and individual health plans, and student health plans, as well as a variety of government-sponsored or government-provided plans.
Is GoodRx considered creditable coverage?
Let’s go back to your initial question, “Why do I need insurance if I can use GoodRx?” GoodRx is NOT insurance. If you have Medicare you have a requirement to be enrolled in an approved (creditable) Prescription Drug Plan. During this time of no coverage you may be able to save money on your medications using GoodRx.
What is not creditable coverage?
“Creditable coverage” means that the prescription drug coverage provided by the group health plan provides benefits that are at least equal to or better than Medicare Part D. “Non-creditable coverage” means that the group health plan’s benefits are less than Medicare prescription drug coverage.
Who gets Medicare creditable coverage notice?
You’ll get this notice each year if you have drug coverage from an employer/union or other group health plan. This notice will let you know whether or not your drug coverage is “creditable.”
What is the evidence of coverage?
The Evidence of Coverage (EOC) is a document that describes in detail the health care benefits covered by the health plan. The EOC can also refer to a certificate or contract provided to a health plan member that contains information about coverage and other rights.
How do I get a creditable coverage certificate?
A Certificate of Creditable Coverage may be obtained from your former health insurance carrier. Please contact your previous health carrier and request them to provide you with a certificate. This certificate may partially or fully apply to your new coverage and alleviate pre-existing situations.
Who gets creditable coverage notice?
A: You must provide a creditable coverage notice to all Medicare eligible individuals who are covered under, or apply for, your prescription drug plan. This requirement applies to active Medicare beneficiaries and those who are retired, as well as Medicare-eligible spouses who are covered as actives or retirees.
How do I know if my prescription drug coverage is ” creditable “?
How do I know if my prescription drug coverage is “creditable”? Your drug plan must tell you each year if your drug coverage is considered creditable coverage. They may send you this information in a letter, or draw your attention to it in a newsletter or other piece of correspondence.
What does it mean for Medicare to have creditable coverage?
The Medicare Modernization Act (MMA) requires entities (whose policies include prescription drug coverage) to notify Medicare eligible policyholders whether their prescription drug coverage is creditable coverage, which means that the coverage is expected to pay on average as much as the standard Medicare prescription drug coverage.
What makes Medicare Part D prescription drug coverage creditable?
A group health plan’s prescription drug coverage is considered creditable if its actuarial value equals or exceeds the actuarial value of standard Medicare Part D prescription drug coverage. Prescription drug coverage that does not meet this standard is called “non-creditable.”
Is it good to have non creditable prescription drug coverage?
Non-creditable prescription drug coverage can still be a valuable benefit for employees. However, individuals need to know whether their prescription drug coverage is creditable or non-creditable.