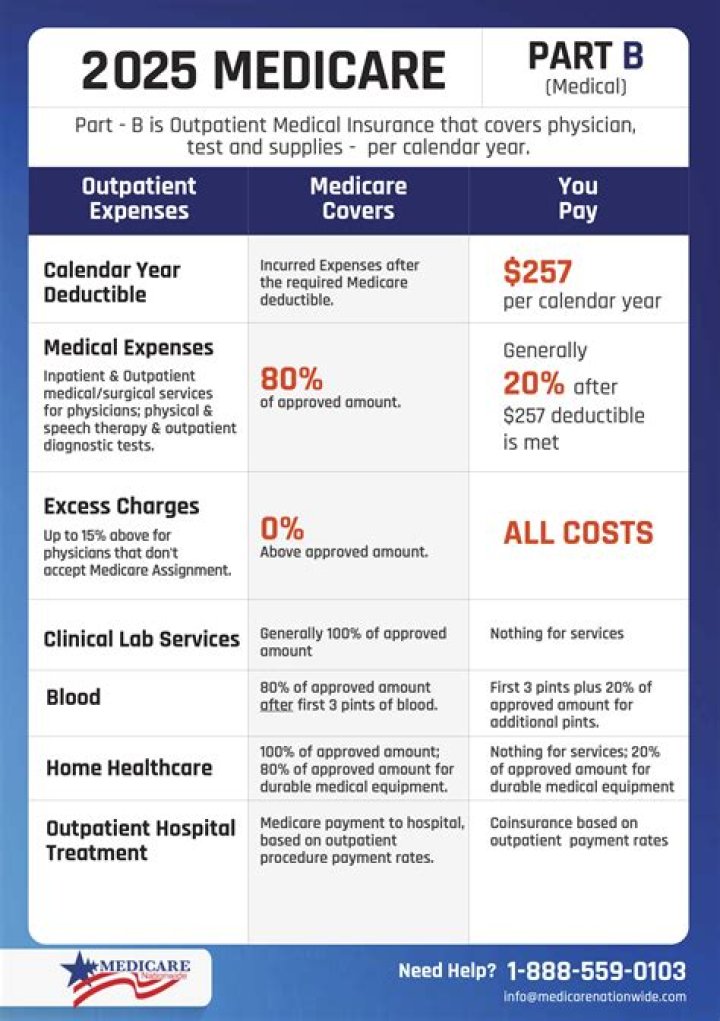
Medicare pays Part B claims (doctors’ services, outpatient hospital care, outpatient physical and speech therapy, certain home health care, ambulance services, medical supplies and equipment) either to your provider or you. For more information, see Assignment for Original Fee-for-Service Medicare .
Is there a cap on Medicare payments?
In general, there’s no upper dollar limit on Medicare benefits. As long as you’re using medical services that Medicare covers—and provided that they’re medically necessary—you can continue to use as many as you need, regardless of how much they cost, in any given year or over the rest of your lifetime.
Which service below is not covered by Part B Medicare?
But there are still some services that Part B does not pay for. If you’re enrolled in the original Medicare program, these gaps in coverage include: Routine services for vision, hearing and dental care — for example, checkups, eyeglasses, hearing aids, dental extractions and dentures.
Can a Dr Bill patient what Medicare did not pay?
This is customary but meaning the balance after Medicare and supplimental pay. I told her the billing clerk is wrong. If a Medicare provider, they must except what Medicare pays. They received 33.77. Bal of 8.44 should have been submitted to supplimental, if not paid then Moms estate will pay the 8.44.
What happens when you become a secondary payer for Medicare?
A secondary payer covers remaining costs, such as coinsurances or copayments. When you become eligible for Medicare, you can still use other insurance plans to lower your costs and get access to more services. Medicare will normally act as a primary payer and cover most of your costs once you’re enrolled in benefits.
Can a hospital refuse to pay a Medicare deductible?
If you have not exhausted your inpatient hospital benefits under Part A, the hospital generally cannot deny treatment or demand payment of your Medicare hospital deductible or copayment. If you have exhausted your covered inpatient days under Part A, the hospital generally may apply the same prepayment policy it has in place for uninsured patients.
What happens when a Medicare provider accepts assignment?
When a provider accepts assignment, they agree to accept Medicare-established fees. Providers cannot bill you for the difference between their normal rate and Medicare set fees. The majority of Medicare payments are sent to providers of Part A and Part B-covered services.